🏥 Improving self-service access to Medicare benefits
Context
Medicare is the federal health insurance program for people who are 65 or older, certain younger people with disabilities, and people with End-Stage Renal Disease. Today, there are over 65,000,000 people on Medicare, and about 12,000,000 of them have online accounts.
CMS provides Medicare.gov accounts to help people on medicare:
Get information about their current benefits.
Understand their out-of-pocket costs.
Take advantage of benefits that keep them healthy and save their out-of-pocket costs.
But, there are various challenges with the current experience that erode trust and reduce adoption. For example:
Users don’t know what to expect from their accounts.
Information provided on the account isn’t specific to a user’s situation.
Medicare jargon prevents users from understanding their benefits.
I lead a team that is working with the Centers for Medicare and Medicaid Services (CMS) to redesign and rebuild the Medicare.gov account experience. At a program level, the problem we’re solving is:
How might we provide self-service experiences that help people on Medicare understand their Medicare benefits and make informed decisions about their Medicare coverage and healthcare?
Our design team includes three UX designers, a content strategist, and me. As the design lead, I am responsible for managing our relationship with CMS, ensuring each team member is positioned for success, guiding our approach, providing strategic direction, and contributing to design deliverables.
How we approached the program
Supporting CMS’ priorities
The Medicare.gov account experience has the attention of a lot of stakeholders from across the organization, so our team must navigate a variety of (sometimes competing) priorities. Some of the higher-level priorities that affect our work include:
Scaling with a growing population – The number of people on Medicare is projected to increase in the coming decade as baby boomers age into the program. To support the growing population, CMS needs more beneficiaries to use self-service tools to manage their benefits so it can scale to support all beneficiaries.
Supporting healthcare decisions – CMS wants to leverage its data to provide personalized experiences that help beneficiaries make informed decisions about their healthcare and benefits.
Adapting to changing priorities – So far, our project has spanned two administrations with very different priorities. The Trump administration prioritized price transparency while the Biden administration is prioritizing health access and equity. Therefore, our approach needs to be able to adapt to ever changing priorities.
Supporting existing users while improving the experience – While we are designing the new experience, we need to maintain the legacy account application. Each change from the legacy to the new experience tends to disrupt current users and decrease overall satisfaction temporarily. Website customer satisfaction is a critical performance metric for our project sponsors.
Evolving the account experience to provide increasingly personalized experiences
We proposed a phased approach that incrementally supports a more holistic, personalized self-service benefits experience for people on Medicare. First, we prioritized the foundational components of the experience (e.g. navigation, messaging, and account home). Then we planned to re-design each of the account features (e.g. claims, preventive services, plans, etc). Finally, we could identify and design cross-feature experiences that help people on Medicare navigate complex coverage and health journeys, like being diagnosed with a chronic condition.
Illustration of how our phased approach would evolve the account experience. Click to enlarge.
The phases of our approach include:
1️⃣ Unifying the navigation across Medicare.gov.
2️⃣ Bringing Medicare to users when they need it with improved messaging.
3️⃣ Guiding users to relevant self-service information with a new account home.
4️⃣ Helping users understand and manage their benefits with improved account feature experiences.
5️⃣ Supporting users through complex care journeys with integrated account features.
Establishing our design operations and processes
To make our work transparent and predictable for CMS stakeholders, we developed and maintained program design operations that define how we work.
The design operations we’ve created have been so successful that CMS now uses our tools and processes for the other programs that support Medicare.gov.
1️⃣ Unifying the navigation across Medicare.gov
The eight Medicare.gov applications are each managed by a separate contracting team. As a result, the experience users had on the website matched the organizational structure of the teams creating the Medicare.gov applications. Users would frequently end up with upwards of five Medicare.gov tabs open when trying to complete a task like, looking up what their current drug plan covers. The problem we were trying to solve was:
How might we help users easily find what they’re looking for no matter where they are on Medicare.gov?
Each application across Medicare.gov had a unique navigation experience.
Co-designing and iterating on the new experience
Before we started on the project, the CMS Division of Research had completed generative research studies to understand how people on Medicare think about their benefits and what they expect Medicare to know about them.
Using their research findings and our insights from our discovery, we facilitated co-design sessions with CMS stakeholders.
In partnership with the CMS Division of Web Experience and the Division of Research, we designed and tested new concepts across three rounds of usability testing with a representative sample of 72 research participants. Our final design allows users to seamlessly navigate all of Medicare.gov whether they are visiting as a guest or they’re logged in.
Examples of the final design shown on three separate application from Medicare.gov. Click to enlarge.
Measuring the new experience
After we released the new experience, we tracked how users' behavior changed, what they were saying about their new experience, and how user satisfaction metrics changed. For example, one quote from a user was:
"I am 74 yrs old, know little about computers, and I find it very easy to navigate on this website and find the information for which I am looking. "
Website survey response from Medicare beneficiary
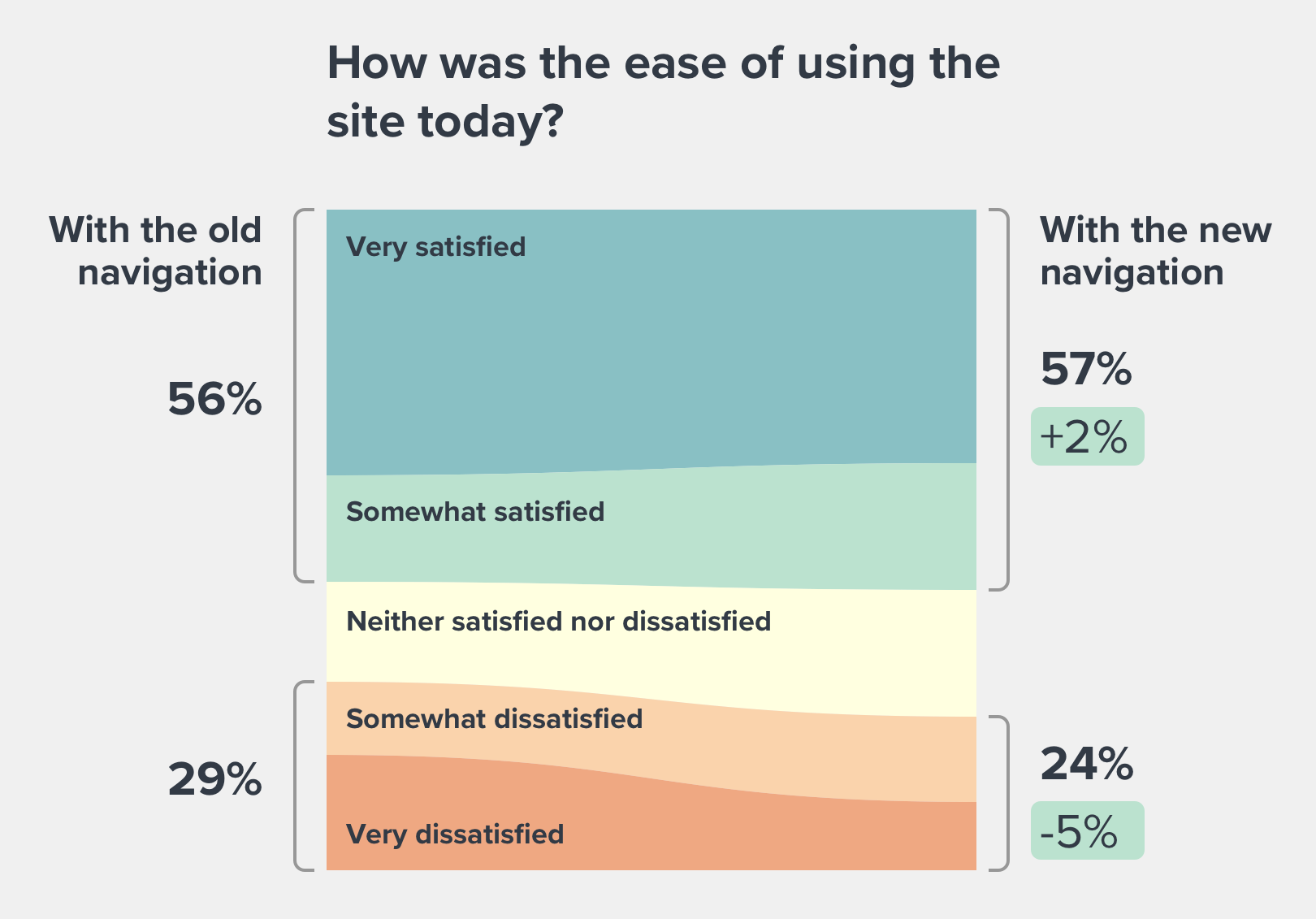
We saw a significant improvement in the ease of use questions from the site-wide customer satisfaction survey.
Using what we learned to improve the rest of the experience
While the new design significantly improved the experience, we found that logged-in users needed to be able to navigate between their account pages more efficiently. We used this insight to design a better home and navigation experience for logged-in users.
2️⃣ Bringing Medicare to users when they need it with improved messaging
The legacy account experience included a message center where users could get messages and corresponding email notifications directly from Medicare. However, the messages and emails Medicare had been sending were generic and often felt like "advertising." Also, CMS had no visibility into the efficacy of its messages. The problem we were trying to solve was:
How might we help users know when there is something important in their Medicare account that needs their attention?
Identifying messages that users want and need
Like in our work with the new consistent navigation, the CMS Division of Research had completed generative research studies to inform our design. They focused on understanding the types of messages users expected, felt were valuable, or that they didn't want from Medicare. Critical insight:
The research found that users are sensitive to messaging from Medicare that contradicts their doctors. Users want messages to help them manage and use their Medicare benefits and avoid mistakes.
Co-designing and iterating on the message center experience
We ran co-design workshops with stakeholders from across CMS to generate new ideas for messages and concepts for the new message center experience.
During our workshops, we focused on ideating new messages in the context of various user journeys.
In partnership with the CMS Division of Web Experience and the Division of Research, we designed and tested new concepts across two rounds of usability testing with a representative sample of 48 research participants. Our research found that a dialog-based message center integrated with the new consistent navigation allowed users to check their messages without losing their place.
Example of the final design integrated with the consistent navigation. Click to enlarge.
Measuring the new experience
After we released the new experience, we tracked how effective each message was at guiding users to valuable content and features. For example, one message prompts users who hadn't done so already to add an authorized representative to their account. Something we know users find important but that they rarely find on their own.
Following the new message, traffic to the authorized representative experience doubled.
Evolving the experience with new, better messages while establishing message governance
The messages we could support at the launch were limited in scope due to data constraints. However, in later phases of the project, as more data were available to the API, we would be able to create increasingly personalized messages that complemented the new account experiences. In addition, shortly after launching the new message center, we developed a message governance process managing messaging ideas. Notifications gating, as we call it, helps CMS strategically plan how and when they message each beneficiary and avoid sending redundant messages across channels.
3️⃣ Guiding users to relevant self-service information with a new account home
The legacy account home provides all users with the same experience, regardless of their situation. For example, one of the primary calls to action on the legacy home page is to "pay my premium," a feature that only applies to 6% of people on Medicare. While it's an essential feature for that 6%, 94% of users see something that doesn't apply to them every time they log in. To make matters worse, this disconnect resulted in anxiety for many users who, upon seeing the prompt, thought that they had been neglecting to pay their premiums! The problem we were trying to solve was:
How might we help beneficiaries quickly understand their benefits and find what they logged in to do?
Example of the legacy account home experience. Click to enlarge.
Understanding how people use their Medicare.gov accounts and what they need when they log in
We started by pulling together relevant data from web analytics, evaluative research studies, in-depth interviews, online survey responses, and call center representative interviews. The diverse data helped us see the legacy experience and user needs from various perspectives.
Co-designing and iterating on the account home experience
We ran co-design workshops with stakeholders from across CMS to generate new ideas for a new account home experience.
During our workshops, we used Invision Freehand to generate a variety of ideas and concepts.
In partnership with the CMS Division of Web Experience and the Division of Research, we designed and tested new concepts across two rounds of usability testing with a representative sample of 35 research participants. For example, our research found that having personalized top-tasks at the top of the page alongside a snapshot of a user's current benefits helped build a clearer expectation for what Medicare.gov could provide. For example, one quote from a user was:
“Anything I’d be looking for is right here. This, to me, makes more sense. It’s more concise. I was drawn to this layout.”
Research participant – current Medicare beneficiary
Example of the final design. Click to enlarge.
Designing for a personalized home page experience
We created a personalization matrix that mapped various user attributes with features available on the new account home experience. The personalization allowed us to communicate how the new experience worked to CMS stakeholders.
Screenshot of the personalization matrix for the new account home experience.
Implementing the new account home
The new account home has not yet been released, but our team is eager to see how the new experience can improve access to critical features and help people manage their Medicare.
4️⃣ Helping users understand and manage their claims
With the foundational and core pieces of the account experience designed, our team shifted our focus to the main features of the account experience. The first feature within the account that we focused on was how people access their Medicare claims. People rely on Medicare claims to understand what they were billed for and what they may need to pay and identify fraud.
While the claims experience is the most commonly visited section of the account, users frequently struggle when using the application. Some of the most persistent issues are:
The layout of the information on the claims details page makes it difficult to see how the various costs add up.
The claims landing page defaults to only showing claims from the past 30 days, so users can be confused if shown a blank list of claims.
Example of the legacy claims experience. Click to enlarge.
Understanding how and when people read their claims and what's important and mapping the claims journey
We observed 24 active users reading their claims using the legacy application during in-depth interviews. These interviews combined with web analytics, online survey responses, and call center representative experiences help us understand users' needs when reviewing their claims and map the claims journey. The most important things for users when looking at their claims are:
What will I need to pay out of pocket?
What did the doctor bill me for?
How much did/didn't Medicare cover?
If Medicare denied something, why?
Co-designing and iterating on the claims experience
In partnership with the CMS Division of Web Experience and the Division of Research, we designed and tested new concepts across two rounds of usability testing with a representative sample of 64 research participants.
Example of the final design. Click to enlarge.
We found that participants benefited from having their deductible contextualized in their claim details so they could better understand what Medicare paid. By showing the math plainly on the page with additional context, participants could more easily understand their claim. For example, one quote from a user was:
"It's got a plus sign, a minus sign, and an equals sign. It breaks down everything. It's easy to read and to pick things out quickly."
Research participant – current Medicare beneficiary
Implementing the new claims experience
The new claims experience has not yet been released, but our team is eager to see how the new experience can improve access to critical features and help people manage their Medicare.
👀 The story isn’t over
Our team continues to work to improve the experience for millions of people on Medicare. I’ll continue adding to this story as our work progresses.